Medical Billing and Coding in 2026: Complete Career Guide and Industry Outlook

The healthcare revenue cycle has transformed dramatically. Medical billing and coding professionals now navigate AI-assisted workflows, value-based reimbursement models, and increasingly complex regulatory requirements that didn’t exist just five years ago.
Table of Contents
ToggleIf you’re considering a career in medical billing and coding or looking to understand how the profession has evolved, you’re facing a landscape where traditional skills meet cutting-edge technology. This guide examines the current state of medical billing and coding, career prospects, required certifications, salary expectations, and the real-world changes reshaping this essential healthcare field.

What Is Medical Billing and Coding in 2026?
Medical billing and coding remains the backbone of healthcare revenue cycle management, but the role has expanded beyond simple code assignment and claim submission.
Medical coding involves translating healthcare diagnoses, procedures, medical services, and equipment into universal alphanumeric codes. Coders use three primary code sets:
- ICD-11-CM (International Classification of Diseases, 11th Revision, Clinical Modification) – diagnostic codes that replaced ICD-10 in late 2023
- CPT (Current Procedural Terminology) – procedure and service codes
- HCPCS (Healthcare Common Procedure Coding System) – codes for supplies, equipment, and services not covered by CPT
Medical billing encompasses submitting claims to insurance companies, following up on payments, managing denials, and ensuring healthcare providers receive proper reimbursement for services rendered.
How the Role Has Changed
The profession has shifted from purely manual code lookup to AI-augmented decision-making. Modern medical coders work alongside natural language processing (NLP) tools that suggest codes from clinical documentation, but human expertise remains essential for:
- Reviewing AI-generated code suggestions for accuracy
- Handling complex, multi-system cases
- Ensuring compliance with payer-specific requirements
- Managing appeals and denials requiring clinical judgment
- Auditing for quality assurance
Current Job Market and Career Outlook
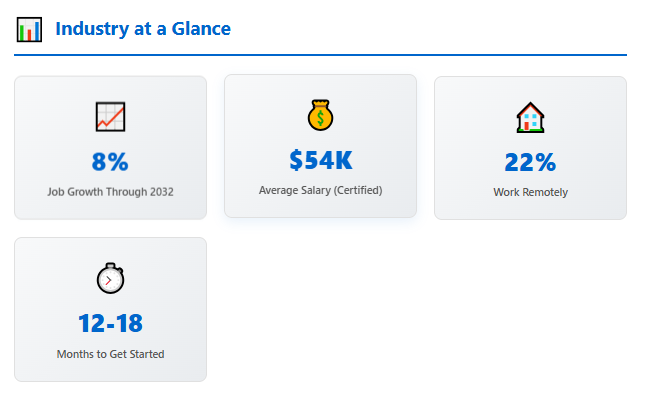
The Bureau of Labor Statistics projects 8% growth for medical records specialists (including billing and coding professionals) through 2032, faster than the average for all occupations. However, the 2026 job market reveals important nuances.
Demand Drivers
Several factors continue fueling demand for skilled billing and coding professionals:
- Aging population: The 65+ demographic requires more healthcare services, generating increased coding volume
- Regulatory complexity: Frequent updates to coding systems, payer policies, and compliance requirements demand specialized expertise
- Value-based care expansion: New reimbursement models require sophisticated coding to capture quality metrics and risk adjustment
- Technology implementation gap: Healthcare organizations need professionals who can bridge clinical documentation and billing technology
Employment Settings
Medical billers and coders work across diverse environments:
| Setting | Percentage of Professionals | Key Characteristics |
|---|---|---|
| Hospitals | 35% | Complex cases, inpatient/outpatient coding, higher compensation |
| Physician offices | 28% | Outpatient focus, specialty-specific coding |
| Remote/home-based | 22% | Growing segment, requires 2+ years experience typically |
| Billing companies | 10% | High volume, multiple clients, productivity metrics |
| Insurance companies | 5% | Claims review, auditing, policy development |
The remote work trend has permanently altered the profession. Most employers now offer hybrid or fully remote positions for experienced coders, though entry-level positions increasingly require on-site training periods of 6-12 months.
Medical Billing and Coding Salaries in 2026
Compensation varies significantly based on certification level, specialization, experience, and geographic location.
National Salary Ranges
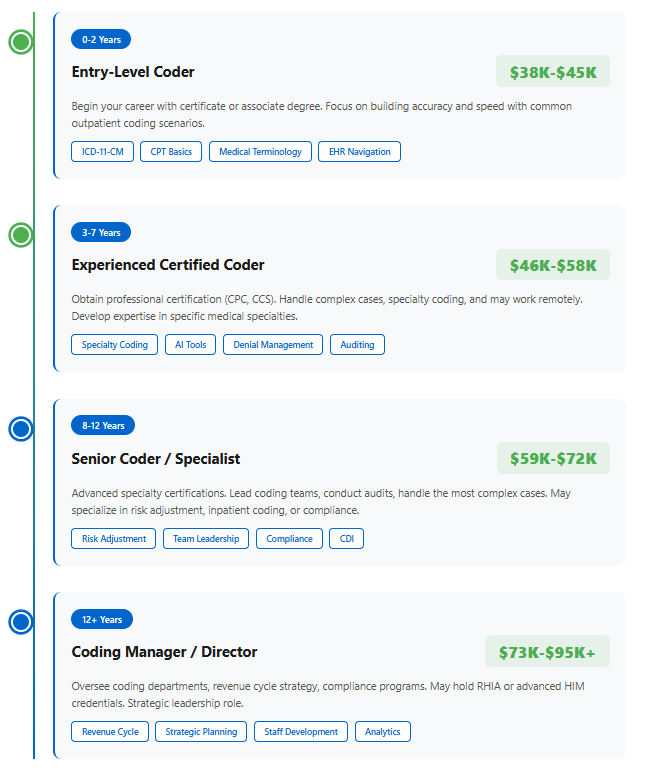
- Entry-level (0-2 years): $38,000 – $45,000
- Mid-career (3-7 years): $46,000 – $58,000
- Experienced (8+ years): $59,000 – $72,000
- Specialized/certified (senior coders, auditors): $73,000 – $95,000
Certification Impact
Certified professionals earn approximately 20-25% more than non-certified counterparts:
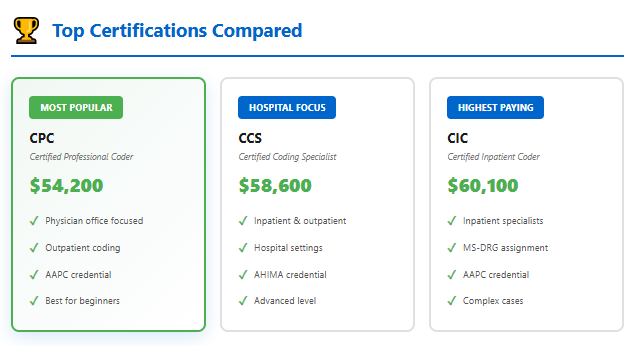
- CPC (Certified Professional Coder): Average $54,200
- CCS (Certified Coding Specialist): Average $58,600
- CCS-P (Certified Coding Specialist-Physician): Average $56,800
- COC (Certified Outpatient Coder): Average $55,400
- CIC (Certified Inpatient Coder): Average $60,100
Specialty certifications command premium compensation. Interventional radiology coders, cardiology coders, and risk adjustment coders often earn $65,000-$80,000 with appropriate credentials and experience.
Geographic Variations
High-cost-of-living areas and states with larger healthcare infrastructure offer higher salaries:
- Top-paying states: California ($62,300 avg), New York ($59,800 avg), Massachusetts ($58,400 avg)
- Remote position advantage: Many professionals in lower-cost states now access higher salaries through remote work with organizations based in premium markets
Education and Certification Requirements
The barrier to entry remains accessible compared to many healthcare professions, but employer expectations have increased.
Educational Pathways
Minimum requirements for most positions:
- High school diploma or GED
- Medical billing and coding certificate or associate degree
- Training programs typically require 9-18 months
Recommended path for competitive candidates:
- Associate degree in Health Information Management or Medical Billing and Coding (2 years)
- Specialized coursework in anatomy, physiology, medical terminology, pharmacology, and healthcare law
- Practicum or externship providing real-world experience
Essential Certifications
AAPC (American Academy of Professional Coders) certifications:
- CPC – The most widely recognized credential, focused on physician office coding
- COC – Outpatient facility coding
- CIC – Inpatient hospital coding
- Specialty certifications – Available for cardiology, orthopedics, emergency medicine, and 20+ other specialties
AHIMA (American Health Information Management Association) credentials:
- CCS – Comprehensive inpatient and outpatient coding, hospital-focused
- CCS-P – Physician-based coding
- RHIA/RHIT – Advanced health information management credentials
Certification Requirements
Most certifications require:
- Passing a comprehensive exam (150-175 questions, 4-5 hours)
- Continuing education (CEUs) for renewal every 1-2 years
- Some require work experience or education prerequisites
Exam pass rates hover around 60-70% for first-time test-takers, making thorough preparation essential.
New Competencies for 2026
Beyond traditional coding knowledge, employers now expect:
- AI tool proficiency: Experience with computer-assisted coding (CAC) software
- Data analytics basics: Understanding of coding metrics, denial patterns, and quality indicators
- Compliance expertise: Knowledge of HIPAA, fraud and abuse regulations, and OIG guidance
- EHR navigation: Facility with major systems (Epic, Cerner/Oracle Health, Meditech)
Technology Reshaping Medical Billing and Coding
Artificial intelligence and automation have fundamentally altered daily workflows without replacing human coders.
AI-Assisted Coding
Natural Language Processing (NLP) tools analyze clinical documentation and suggest appropriate codes. Current systems achieve approximately 85-92% accuracy for routine cases, but human review remains mandatory.
Coders now spend their time:
- 30-40% reviewing and validating AI suggestions
- 25-30% coding complex cases requiring clinical judgment
- 20-25% managing queries to providers for documentation clarification
- 10-15% auditing and quality assurance
Automation in Billing
Revenue cycle management platforms automate:
- Eligibility verification and pre-authorization requests
- Claim scrubbing for common errors before submission
- Electronic claim submission and status tracking
- Payment posting and reconciliation
- Denial pattern identification
This automation shifts billing specialists toward exception management – handling denials, appeals, complex claims, and patient billing inquiries that require human expertise.
Blockchain and Claims Processing
Some large payers and health systems are piloting blockchain-based claims adjudication, promising to reduce processing time from days to minutes. Early adopters report 40-50% reduction in administrative costs, though widespread implementation remains 3-5 years away.
Specialization Opportunities
Specializing in specific medical disciplines or coding functions can significantly enhance career prospects and earning potential.
High-Demand Specialties
Interventional procedures: Cardiology, interventional radiology, and pain management coding require advanced knowledge of complex procedures and often involve multiple code assignments per encounter.
Risk adjustment coding: Medicare Advantage and other value-based programs depend on accurate diagnosis coding to determine reimbursement. Risk adjustment coders review documentation to ensure all relevant diagnoses are captured.
Inpatient coding: Hospital coders assign MS-DRGs (Medicare Severity Diagnosis Related Groups) that determine facility reimbursement. This specialty requires understanding of present-on-admission indicators, principal diagnosis selection, and complex coding guidelines.
Emergency medicine: High-volume, time-sensitive coding with diverse case mix and frequent E/M level determination.
Functional Specializations
Beyond medical specialties, coders can specialize in specific functions:
- Auditing: Reviewing coded records for accuracy, compliance, and revenue optimization
- CDI (Clinical Documentation Improvement): Working with physicians to enhance documentation quality
- Denial management: Analyzing denials, working appeals, and identifying systemic issues
- Compliance: Ensuring adherence to coding guidelines, payer policies, and regulatory requirements
- Education: Training new coders and providing ongoing education
Challenges Facing Medical Billing and Coding Professionals
Understanding current challenges helps you prepare for the realities of the profession.
Regulatory Complexity
The coding and billing regulatory environment grows more complex annually:
- Quarterly CPT updates and annual ICD-11-CM changes
- Payer-specific policies that vary for the same procedure across different insurance companies
- Compliance requirements including modifier usage, medical necessity, and documentation standards
- Evolving fraud and abuse regulations under the False Claims Act
Denial Rates and Revenue Cycle Pressure
Healthcare organizations face increasing pressure to reduce claim denials and accelerate payment. Initial denial rates average 15-20% across the industry, with complex cases seeing higher rates.
Billing and coding professionals must navigate:
- Increasingly stringent medical necessity requirements
- Prior authorization complexities
- Frequent payer policy changes
- Documentation gaps requiring provider queries
Transition to Value-Based Care
The shift from fee-for-service to value-based reimbursement models requires coders to:
- Understand quality measure coding and reporting
- Capture comprehensive diagnosis lists for risk adjustment
- Code social determinants of health (SDOH)
- Support population health analytics through accurate data capture
Burnout and Productivity Pressure
High-volume production expectations can lead to burnout. Many organizations expect:
- Outpatient coders: 40-60 encounters per day
- Inpatient coders: 15-25 charts per day
- Quality accuracy scores: 95%+ required
Balancing speed and accuracy remains a persistent challenge.
Remote Work: Opportunities and Considerations
Remote medical coding has become standard, but it comes with specific considerations.
Advantages of Remote Coding
- Geographic flexibility: Access opportunities nationwide regardless of location
- Work-life balance: Elimination of commute time and scheduling flexibility
- Expanded opportunities: Work for prestigious health systems or specialized practices without relocating
- Cost savings: Reduced transportation, meal, and wardrobe expenses
Remote Work Requirements
Employers typically require:
- Minimum experience: 2+ years of coding experience
- Productivity benchmarks: Meet or exceed productivity standards
- Technology setup: Reliable high-speed internet, dedicated workspace, often dual monitors
- Availability: Scheduled core hours for team meetings and provider queries
- Accuracy metrics: Maintain quality scores above 95%
Challenges of Remote Work
- Isolation: Limited colleague interaction and informal learning opportunities
- Technology dependence: Internet outages directly impact productivity
- Home workspace setup: Ergonomic considerations and dedicated space requirements
- Self-discipline: Time management without office structure
Career Advancement Pathways
Medical billing and coding can serve as a foundation for diverse healthcare career trajectories.
Vertical Advancement
Traditional progression:
- Entry-level coder → Experienced coder
- Senior coder/specialist → Coding supervisor
- Coding manager → Revenue cycle manager
- Director of HIM or Revenue Cycle
Timeline: Progression to management typically requires 5-7 years of coding experience plus leadership development.
Lateral Opportunities
Your coding foundation can transition to:
- Clinical Documentation Improvement Specialist: Work with physicians to improve documentation (often requires clinical background)
- Healthcare Compliance Officer: Focus on regulatory adherence
- Revenue Cycle Analyst: Data analysis and process improvement
- Practice Management: Oversee overall office operations
- Medical Coding Educator: Train the next generation of coders
- Consultant: Independent or firm-based consulting for coding optimization
Advanced Credentials
RHIA (Registered Health Information Administrator) or RHIT (Registered Health Information Technician) credentials from AHIMA open doors to broader health information management roles, often requiring a bachelor’s degree.
Coding certifications in multiple specialties demonstrate versatility and command higher compensation.
How to Start Your Medical Billing and Coding Career
A strategic approach to entering the field increases your chances of securing desirable positions.
Step 1: Choose Your Training Program
Select an AAPC-approved or AHIMA-approved program to ensure quality education and certification eligibility. Consider:
- Program length: Certificate (9-12 months) vs. associate degree (2 years)
- Format: In-person, online, or hybrid
- Externship opportunities: Hands-on experience significantly improves job prospects
- Certification exam preparation: Built-in exam prep and vouchers
- Cost: Ranges from $1,200-$15,000 depending on format and institution
Step 2: Gain Practical Experience
During training:
- Complete all practicum or externship opportunities
- Use practice coding software extensively
- Join student chapters of professional organizations
- Practice with real case studies and coding scenarios
Entry-level opportunities:
- Medical records clerk positions in healthcare facilities
- Front office positions in physician practices
- Billing support roles in healthcare organizations
These adjacent positions provide healthcare environment exposure while you complete certification.
Step 3: Obtain Certification
Timing: Most candidates sit for certification exams immediately after completing training or within 6 months.
Preparation:
- Utilize study guides, practice exams, and review courses
- Join study groups through AAPC or AHIMA local chapters
- Budget 100-150 hours of dedicated exam preparation
- Invest in official code books with tabs and annotations
First-time certification costs (typical):
- AAPC membership: $220/year
- CPC exam: $460
- Study materials: $200-400
- Total: ~$900-1,100
Step 4: Build Your Resume and Apply Strategically
Entry-level applicants should emphasize:
- Certification credentials prominently
- Specific coding systems knowledge (ICD-11-CM, CPT, HCPCS)
- Externship or practicum experience with measurable accomplishments
- Technical proficiencies (EHR systems, coding software)
- Accuracy metrics from training exercises
Application strategy:
- Start with larger healthcare systems that have structured training programs
- Consider temporary or contract positions to gain experience
- Network through AAPC and AHIMA local chapter meetings
- Target positions explicitly marked as “entry-level” or “apprentice”
Frequently Asked Questions
Is medical billing and coding still in demand in 2026?
Yes, medical billing and coding remains in strong demand despite automation advances. The Bureau of Labor Statistics projects 8% growth through 2032. While AI tools handle routine coding tasks, healthcare organizations need skilled professionals to manage complex cases, ensure compliance, work denials, and bridge technology with clinical documentation. The role has evolved rather than disappeared, with emphasis shifting to quality review, exception handling, and specialized coding.
Can you work from home as a medical biller or coder?
Remote work is now standard in medical billing and coding, with approximately 22% of professionals working fully remotely and many others in hybrid arrangements. However, most employers require 2+ years of experience, proven productivity, and quality metrics before offering remote positions. Entry-level coders typically need 6-12 months of on-site training. Remote positions require reliable internet, dedicated workspace, and the ability to meet productivity benchmarks independently.
How much does medical billing and coding certification cost?
Initial certification costs range from $900-$1,100, including professional association membership ($220), exam fees ($400-460), and study materials ($200-400). Training programs cost $1,200-$15,000 depending on certificate vs. degree format. Certifications require renewal every 1-2 years with continuing education units, averaging $200-300 annually. While certification isn’t legally required, 85%+ of employers require or strongly prefer certified candidates, and certified professionals earn 20-25% more.
What’s the difference between medical billing and medical coding?
Medical coding translates clinical documentation into standardized alphanumeric codes (ICD-11-CM for diagnoses, CPT for procedures) that describe what conditions were treated and what services were provided. Medical billing uses those codes to create and submit claims to insurance companies, follow up on payments, manage denials, and handle patient billing. Many positions combine both functions, though larger organizations may separate roles. Coding requires more detailed clinical knowledge, while billing emphasizes payer policies and revenue cycle management.
Will AI replace medical coders?
AI will not replace medical coders but is transforming the role significantly. Current AI-assisted coding achieves 85-92% accuracy on routine cases but struggles with complex scenarios requiring clinical judgment, documentation interpretation, and regulatory knowledge. The profession is shifting from manual code lookup to AI suggestion review, complex case management, quality auditing, and compliance oversight. Employment projections show continued growth, with demand shifting toward professionals who can work effectively with AI tools while providing the expert judgment automation cannot replicate.
How long does it take to become a certified medical coder?
Most professionals complete training and certification in 12-18 months. A certificate program requires 9-12 months, while an associate degree takes two years. After completing education, candidates typically spend 2-3 months preparing for certification exams. The total timeline from starting education to securing employment usually spans 15-24 months. Accelerated programs exist but may not provide sufficient preparation. Some candidates complete online self-study programs in 6-9 months, though structured programs with instructor support typically produce better outcomes and higher first-time pass rates.
Summary: The Future of Medical Billing and Coding
Medical billing and coding in 2026 offers a stable, accessible healthcare career path with clear advancement opportunities and increasing remote work options. The profession has evolved significantly, requiring professionals who can work alongside AI tools while providing the clinical judgment, compliance expertise, and complex problem-solving that technology cannot replicate.
Key takeaways:
The role combines technology proficiency with healthcare knowledge, making it resistant to complete automation. Certification through AAPC or AHIMA significantly improves employment prospects and earning potential. Specialization in high-demand areas like risk adjustment, inpatient coding, or specific medical specialties can accelerate career growth.
Entry requires modest educational investment (12-18 months) compared to many healthcare careers, with certification costs around $900-$1,100. Salaries range from $38,000 for entry-level positions to $95,000+ for specialized senior roles. Remote work opportunities have expanded permanently, though most require proven experience.
The shift toward value-based care, continued regulatory complexity, and healthcare’s digital transformation ensure ongoing demand for skilled billing and coding professionals who can adapt to evolving technology while maintaining the accuracy and compliance standards essential to healthcare revenue cycle success.